The surveys provided a great snapshot of practice pharmacists work at the time but this is an area which has seen rapid change. We therefore plan to send out a new survey to pharmacists currently working in general practice to see how things have changed. We hope to be able to provide an update on how things have changed later in the year.
The response was excellent with over 900 respondents in total and was broadly representative of populations across the four nations of the UK implying a wide distribution. Below are some of the results.
Experience
More than 98% of pharmacists had been registered for more than 3 years. However, 56% had only been working in general practice for less than two years. These pharmacists have predominantly come from the community and hospital sectors. Crucially, although there is some ongoing portfolio working, many are not continuing to work in those sectors.
Fig. 1 Cross Sector Working
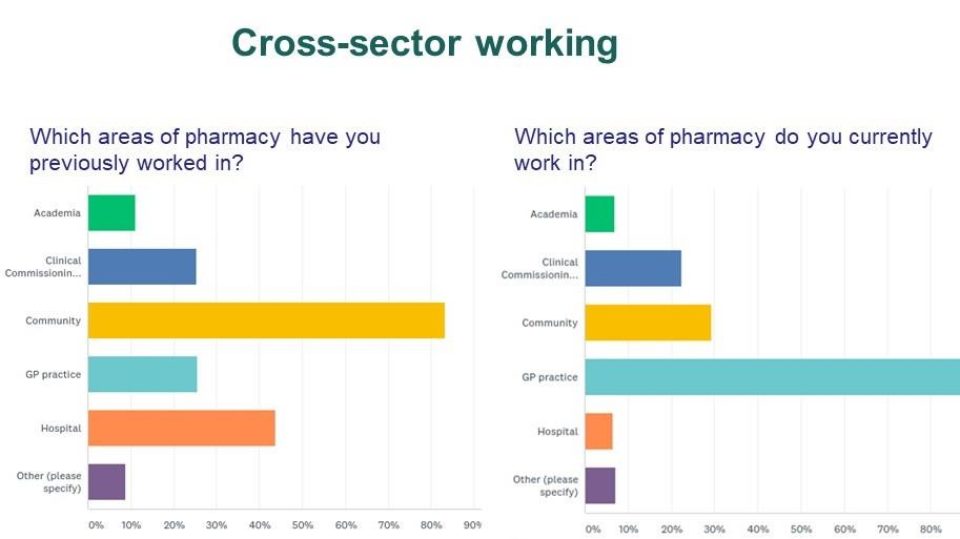
In England, 45% of the respondents to this survey who were not part of the NHSE pilot have only been in GP for less than 2 years. This would indicate that there have been large numbers of pharmacists moving into general practice outside of the NHSE program.
Work Patterns & Employment Status
Table 1 summarises some key differences around work patterns and employment status between the countries. Some of this can be explained by the differences in the recent national NHS funding schemes, whilst also reflecting a greater use of established practice pharmacists prior to 2015 in certain countries.
Table 1. Summary of variation in Employment status and work patterns across the UK
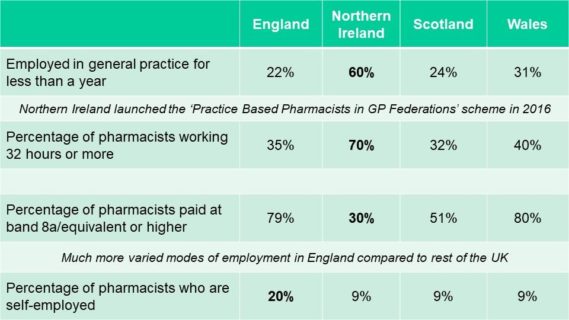
In Northern Ireland, where the Practice Based Pharmacists funding was launched in 2016, 60% of pharmacists had only been in general practice for less than year. It is also the nation with lowest levels of pay (69% at Band 7 level), compared to respondents from England and Wales having significantly larger proportions of pharmacists paid at band 8a rates or higher.
In England, levels of self-employment were much higher in England and indeed employment status was much more variable compared to the rest of the UK (Fig 2). Most pharmacists in Northern Ireland, Scotland and Wales are employed by primary care organisations (PCO) such as Health Boards or Federations. In England the picture is much more varied: as well as a significantly higher proportion of self-employed pharmacists, just under half are employed directly by GP practices, with the rest either self-employed, employed by a PCO, or a non-NHS employer. In fact, private, non-NHS employment was 7% in England and negligible in the rest of the UK.
Fig. 2 Employment status – variation across the UK
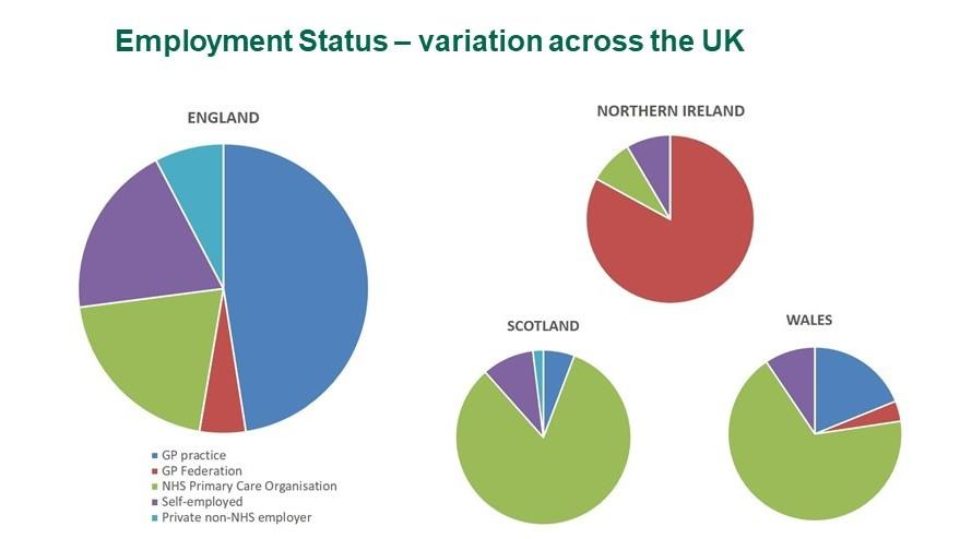
Working under a large organisational structure will provide a governance, clinical supervision and training framework, as well as a more easily accessible network of GP pharmacists thus reducing the risk of isolation, a theme touched on by several respondents who left comments.
“I do not feel adequately supported or trained to undertake the new roles expected of me”
“I am self-employed and feel very isolated as I don’t know anyone locally”
“I have never had any supervision or guidance”
What are pharmacists doing in practice? And what is considered to be most value?
Survey respondents were asked to tick from a comprehensive list of possible services that a pharmacist might do. The results were similar from both the survey of GP pharmacists and that of practice staff (Fig. 3). Most commonly provided services were related to medicines-related activities. The lowest scoring areas were those around diagnosis such as common illness and triage. There also appears to be some ignorance around what general practice staff know about their pharmacist’s role, with GP staff under reporting activities compared to pharmacists.
Fig. 3. What regular services are pharmacists providing their GP practice(s)
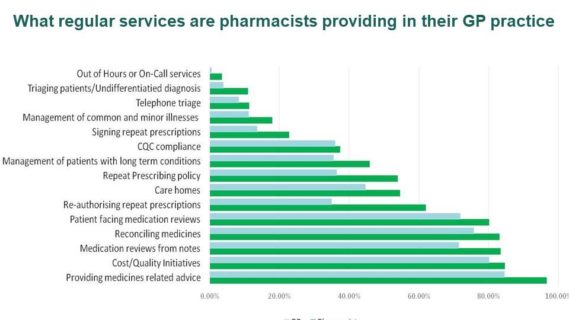
Respondents were asked to rank the services in order of the top 3 that they considered to be of most value to the practice. The results are summarised in table 2 and these show that the pharmacist role was most valued around aspects of pharmaceutical care such as medicines related activities and managing patients with long-term conditions and those of least value were areas involving diagnosis.
Table 2. Services considered of most and least value to the practice
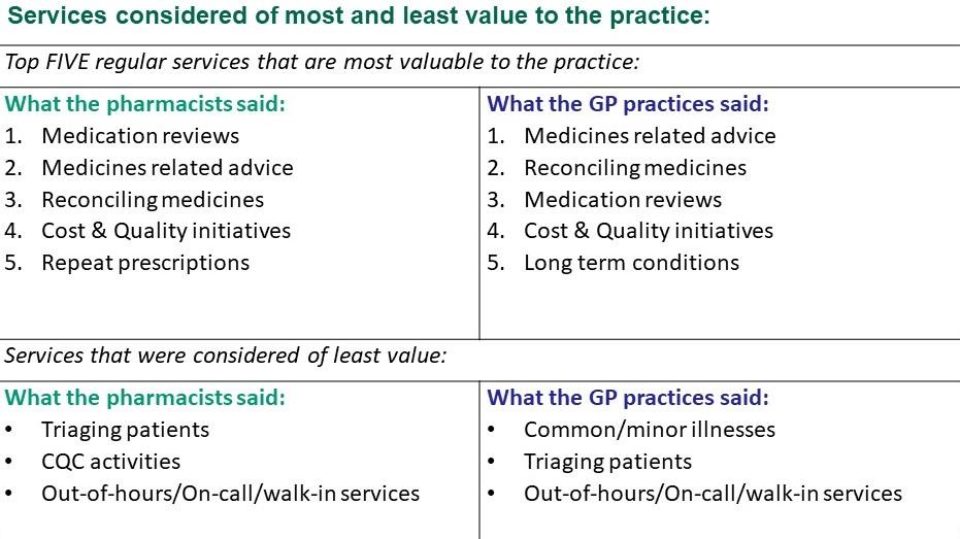
A GP commented: “It is more efficient to make use of pharmacists’ medication related skills as there is a significant workload that can be taken over from GPs. I do not believe that training in areas such as triage or minor illness is a good use of their skills”
The survey results would suggest that pharmacists are doing, and building on, what essentially, they’ve always done in general practice albeit with an evolving increase in clinical skills and patient facing services. But still around pharmaceutical care aspects rather than diagnosing.
Table 3. How are pharmacists getting on in the role?

Perceptions of how pharmacists are getting on in practice
There was a consensus from the survey that advancement of pharmacists in general practice is, on the whole, positive and needs to be continued and developed. Pharmacists are perceived as a positive addition to the team by patients and surgery staff; the role is meeting expectations for many; and, there is confidence in the pharmacist’s abilities. There were lower levels of satisfaction with regard to improving joined up working between sectors and fully utilising the pharmacist’s skills. The relatively low level of satisfaction with governance and supervision was similar across the UK irrespective of being part of a national NHS program.
Salary
Level of pay was a significant concern. 53% of pharmacists did not feel that their current level of pay was appropriate to the job role. There were many comments about this issue, particularly the fact that salaries did not increase correspondingly to extra responsibilities and acquired skills as the pharmacist developed.
“My role and responsibilities have expanded massively since I first started, but my pay hasn’t”
“We will have a pivotal role in delivering patient care, for example managing long term conditions, but there is no increased pay for this”
Long-term funding
How practice pharmacists will be funded over the long-term was raised by pharmacists and GP staff. It was interesting that whilst 87% of GP staff felt there was a long-term future for GP pharmacists, only 30% thought this was feasible without NHS funding, and a further23% weren’t sure.
GP: “I think the tapered funding provided by the scheme is too restrictive and there should be more commitment from NHSE”
Practice Manager: “Pharmacists are a valuable addition to the practice workforce, but funding needs to be provided to ensure a more active role in primary care”
Summary
This survey offers a much-need insight into what pharmacists across the UK are doing in general practice and how they are getting on. Overall, the response was positive and reinforces a widely acknowledged perception that pharmacists are a valuable asset to general practice and are continuing to develop roles that began to be established as far back as the 1990s.
There are, however, a few areas of concern:
- The potential for pharmacists to feel isolated, especially when working in the absence of an overarching supervision and governance framework, and without a structured education and training programme. This is particularly important in the context of increasing numbers of inexperienced pharmacists moving into general practice.
- Impact on the workforce across pharmacy sectors: There are large numbers of pharmacists moving from community and hospital into general practice across the UK. NHSE has committed to funding an extra 1,500 clinical pharmacists by 2020/21 and our survey has demonstrated that there are many more pharmacists being employed outside of the nationally funded program.
- There are high levels of dissatisfaction with regard to salary. The PDA would like to see a more comprehensive structured career framework in place that is linked to a skills and salary escalator thus ensuring that pharmacists are rewarded appropriately as they develop.
- Long term funding: The survey has demonstrated that pharmacists are expanding their unique skillset around pharmaceutical care to great benefit in general practice, and this is being well-received by the surgeries. Development of this role requires sufficient investment. Currently models across the UK vary, with key differences in outlook, vision and levels of financial commitment.